Renal pelvis or ureter cancer
Definition
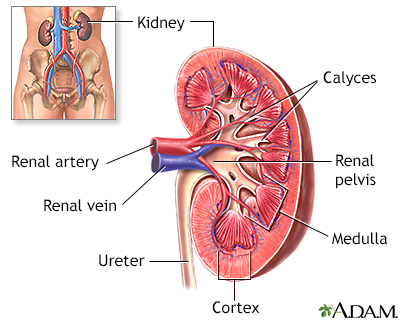
Cancer of the renal pelvis or ureter is cancer that forms in the kidney's pelvis or the tube (ureter) that carries urine from the kidney to the bladder.
Alternative Names
Transitional cell cancer of the renal pelvis or ureter; Kidney cancer - renal pelvis; Ureter cancer; Urothelial carcinoma
Causes
Cancer can grow in the urine collection system, but it is uncommon. Renal pelvis and ureter cancers affect men more often than women. These cancers are more common in people older than 65.
The exact causes of this cancer are not known. Long-term (chronic) irritation of the kidney from harmful substances removed in the urine may be a factor. This irritation may be caused by:
- Kidney damage from medicines, especially ones for pain (analgesic nephropathy)
- Exposure to certain dyes and chemicals used to manufacture leather goods, textiles, plastics, and rubber
- Smoking
People who have had bladder cancer are also at risk.
Symptoms
Symptoms may include any of the following:
- Constant back pain
- Blood in the urine
- Burning, pain, or discomfort with urination
- Fatigue
- Flank pain
- Unexplained weight loss
- Loss of appetite
- Anemia
- Urinary frequency or urgency
Exams and Tests
The health care provider will perform a physical exam, and examine your belly area (abdomen). In rare cases, this may reveal an enlarged kidney.
If tests are done:
- Urinalysis may show blood in the urine.
- A complete blood count (CBC) may show anemia.
- Urine cytology (microscopic examination of cells) may reveal cancer cells.
Other tests that may be ordered include:
- Abdominal CT scan
- Chest x-ray
- Cystoscopy with ureteroscopy
- Intravenous pyelogram (IVP)
- Kidney ultrasound
- MRI of the abdomen
- Renal scan
These tests may reveal a tumor or show that the cancer has spread from the kidneys.
Treatment
The goal of treatment is to eliminate the cancer.
The following procedures may be used to treat the condition:
- Nephroureterectomy -- This involves removal of entire kidney, ureter, and the bladder cuff (tissue that connects ureter to the bladder)
- Nephrectomy -- Surgery to remove all or part of the kidney is often done. This may include removing part of the bladder and tissues around it, or the lymph nodes.
- Ureter resection -- Surgery to remove part of the ureter that contains cancer, and some healthy tissue around it. This may be used in case of superficial tumors present in lower part of the ureter near the bladder. This may help to preserve the kidney.
- Chemotherapy -- This is used when the cancer has spread outside of the kidney or ureter. Because these tumors are similar to a form of bladder cancer, they are treated with a similar type of chemotherapy.
- Immunotherapy -- This is used when the cancer has spread outside of the kidney or ureter. Because these tumors are similar to a form of bladder cancer, they are treated with a similar type of immunotherapy.
Support Groups
You can ease the stress of illness by joining a cancer support group. Sharing with others who have common experiences and problems can help you not feel alone.
Outlook (Prognosis)
Outcome varies, depending on the location of the tumor and whether the cancer has spread. Cancer that is only in the kidney or ureter may be cured with surgery.
Cancer that has spread to other organs is usually not curable.
Possible Complications
Complications from this cancer may include:
- Kidney failure
- Local spread of the tumor with increasing pain
- Spread of the cancer to lung, liver, and bone
When to Contact a Medical Professional
Contact your provider if you have any of the symptoms listed above.
Prevention
Measures that may help prevent this cancer include:
- Follow your provider's advice regarding medicines, including over-the-counter pain medicine.
- Stop smoking.
- Wear protective equipment if you are likely to be exposed to substances that are toxic to the kidneys.
Gallery
References
Bajorin DF. Tumors of the kidney, bladder, ureters, and renal pelvis. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 187.
National Cancer Institute website. Transitional cell cancer of the renal pelvis and ureter treatment (pdq)–health professional version. www.cancer.gov/types/kidney/hp/transitional-cell-treatment-pdq. Updated January 30, 2020. Accessed June 24, 2022.
Wong WW, Daniels TB, Peterson JL, Tyson MD, Tan WW. Kidney and ureteral carcinoma. In: Tepper JE, Foote RL, Michalski JM, eds. Gunderson & Tepper's Clinical Radiation Oncology. 5th ed. Philadelphia, PA: Elsevier; 2021:chap 64.
