Are You at Risk of a Hernia?
Almost everyone has heard of a hernia, but few understand its potential risks. Over five million people in the United States will suffer from a hernia, yet…

Update your location to show providers, locations, and services closest to you.
Gynecologic surgeons at the UF Health are proud to utilize the most advanced robotic technology in the world.
Two da Vinci Si robotic systems are housed at UF Health and are used routinely for a myriad of gynecologic procedures such as hysterectomy, myomectomy, sacrocolpopexy and adnexal surgery. The da Vinci system provides superior 3-D quality visualization and magnification, along with the precision afforded with its unique wristed instruments. Robotic and minimally-invasive approaches offer significant benefits over traditional open surgery, such as less surgical blood loss, less scarring, less pain, better cosmetic results and faster recovery and return to regular activities. Most patients are able to leave the hospital within 24 hours.
Robotic surgery entails the use of small incisions to introduce miniature wristed instruments and a high-definition 3D camera. The surgeon sits at a nearby console, controlling the movements and actions of the miniature instruments inside of the pelvic cavity, while viewing a magnified 3D image of the target organs.”
Almost everyone has heard of a hernia, but few understand its potential risks. Over five million people in the United States will suffer from a hernia, yet…

December 7, 2022
University of Florida Health became one of the first large academic health centers in the Southeast this year to begin using a robot-assisted system in total…
College of Medicine, UF Health Orthopaedics and Sports Medicine Institute, +2 more
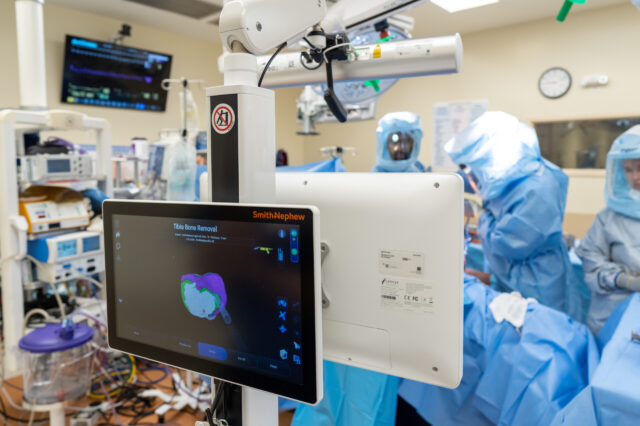
Robotic surgery used to conjure images of science fiction and outer space. But now the use of robots to...