Definition
Muscular dystrophy is a group of inherited disorders that cause muscle weakness and loss of muscle tissue, which get worse over time.
Causes
Muscular dystrophies, or MD, are a group of inherited conditions. This means they are passed down through families. They may occur in childhood or adulthood. There are many different types of muscular dystrophy. They include:
Symptoms
Muscular dystrophy can affect adults, but the more severe forms tend to occur in early childhood.
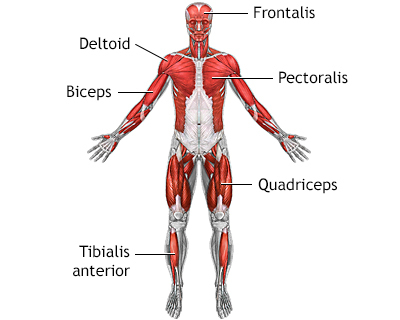
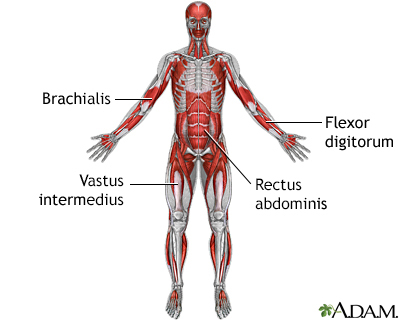
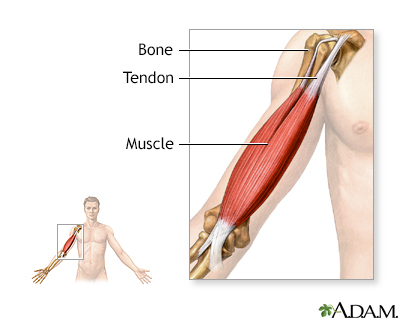
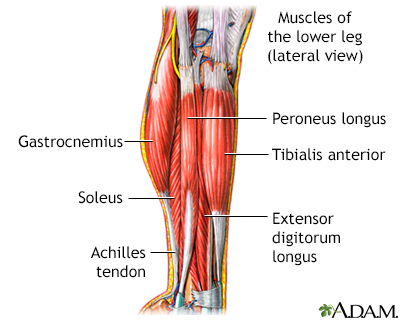
Symptoms vary among the different types of muscular dystrophy. All of the muscles may be affected. Or, only specific groups of muscles may be affected, such as those around the pelvis, shoulder, or face. The muscle weakness slowly gets worse and symptoms can include:
- Delayed development of muscle motor skills
- Difficulty using one or more muscle groups
- Drooling
- Eyelid drooping (ptosis)
- Frequent falls
- Loss of strength in a muscle or group of muscles as an adult
- Loss in muscle size
- Problems walking (delayed walking)
Intellectual disability is present in some types of muscular dystrophy.
Exams and Tests
A physical examination and your medical history will help the health care provider determine the type of muscular dystrophy. Specific muscle groups are affected by different types of muscular dystrophy.
The exam may show:
- Weakness of certain muscles
- Abnormally curved spine (scoliosis)
- Joint contractures (clubfoot, claw-hand, or others)
- Low muscle tone (hypotonia)
Some types of muscular dystrophy involve the heart muscle, causing cardiomyopathy or abnormal heart rhythm (arrhythmia).
Often, there is a loss of muscle mass (wasting). This may be hard to see because some types of muscular dystrophy cause a buildup of fat and connective tissue that makes the muscle appear larger. This is called pseudohypertrophy.
A muscle biopsy may be used to confirm the diagnosis. In some cases, a DNA blood test may be all that is needed.
Other tests may include:
- Heart testing -- electrocardiography (ECG)
- Nerve testing -- nerve conduction and electromyography (EMG)
- Urine and blood testing, including CPK level
- Genetic testing for some forms of muscular dystrophy
- Muscle biopsy
Treatment
There are no known cures for the various muscular dystrophies. The goal of treatment is to control symptoms.
Physical therapy may help maintain muscle strength and function. Leg braces and a wheelchair can improve mobility and self-care. In some cases, surgery on the spine or legs may help improve function.
Corticosteroids taken by mouth are sometimes prescribed to children with certain muscular dystrophies to keep them walking for as long as possible.
The person should be as active as possible. No activity at all (such as bedrest) can make the disease worse.
Some people with breathing weakness may benefit from devices to assist breathing.
Support Groups
You can ease the stress of illness by joining a support group where members share common experiences and problems.
Outlook (Prognosis)
The severity of disability depends on the type of muscular dystrophy. All types of muscular dystrophy slowly get worse, but how fast this happens varies widely.
Some types of muscular dystrophy, such as Duchenne muscular dystrophy in boys, are deadly. Other types cause little disability and people have a normal lifespan.
Prevention
Genetic counseling is advised when there is a family history of muscular dystrophy. Women may have no symptoms, but still carry the gene for the disorder. Duchenne muscular dystrophy can be detected with about 95% accuracy by genetic studies done during pregnancy.
References
Bharucha-Goebel DX. Muscular dystrophies. In: Kliegman RM, St. Geme JW, Blum NJ, Shah SS, Tasker RC, Wilson KM, eds. Nelson Textbook of Pediatrics. 21st ed. Philadelphia, PA: Elsevier; 2020:chap 627.
Selcen D. Muscle diseases. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 393.