Acid Reflux Ties to Esophageal Cancer
Gastroesophageal reflux disease, or GERD, may have links to esophageal cancer. GERD is a condition in which stomach acid leaks into your esophagus, or food…

Update your location to show providers, locations, and services closest to you.
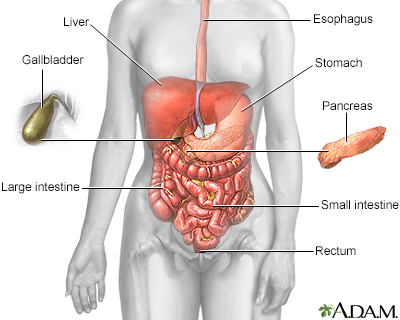
Barrett esophagus (BE) is a disorder in which the lining of the esophagus is damaged by stomach acid. The esophagus is also called the food pipe, and it connects your throat to your stomach.
People with BE have an increased risk for cancer in the area involved. However, cancer is not common.
Barrett's esophagus; GERD - Barrett; Reflux - Barrett
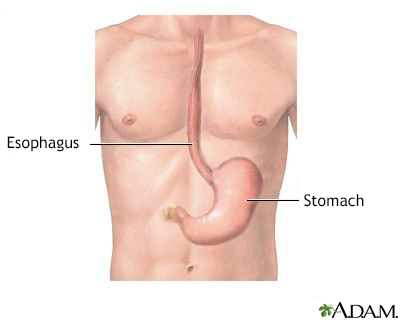
When you eat, food passes from your throat to your stomach through the esophagus. A ring of muscle fibers in the lower esophagus keeps stomach contents from moving backward.
If these muscles do not close tightly, harsh stomach acid can leak into the esophagus. This is called reflux or gastroesophageal reflux (GERD). It may cause tissue damage over time. The lining becomes similar to that of the stomach.
BE occurs more often in men than women. People who have had GERD for a long time are more likely to have this condition.
BE itself does not cause symptoms. The acid reflux that causes BE often leads to symptoms of heartburn. Many people with this condition do not have any symptoms.
You may need an endoscopy if GERD symptoms are severe or come back after treatment.
During the endoscopy, your endoscopist may take tissue samples (biopsies) from different parts of the esophagus. These samples help detect the condition. They also help look for changes that could lead to cancer.
Your provider may recommend a follow-up endoscopy to look for cell changes that indicate cancer at regular intervals.
TREATMENT OF GERD
Treatment should improve acid reflux symptoms, and may keep BE from getting worse. Treatment may involve lifestyle changes and medicines such as:
Lifestyle changes, medicines, and anti-reflux surgery may help with symptoms of GERD. However, these steps will not make BE go away.
TREATMENT OF BARRETT ESOPHAGUS
Endoscopic biopsy can show changes in the cell that may be cancer. You provider may advise surgery or other procedures to treat it.
Some of the following procedures remove the harmful tissue in your esophagus:
Treatment should improve acid reflux symptoms and may keep BE from getting worse. None of these treatments will reverse the changes that may lead to cancer.
People with chronic GERD or Barrett esophagitis generally need to be monitored for cancer of the esophagus.
Contact your provider if:
Early detection and treatment of GERD may prevent BE.
Falk GW, Katzka DA. Diseases of the esophagus. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 129.
Jackson AS, Louie BE. Management of Barrett's esophagus. In: Cameron AM, Cameron JL, eds. Current Surgical Therapy. 13th ed. Philadelphia, PA: Elsevier; 2020:19-25.
Ku GY, Ilson DH. Cancer of the esophagus. In: Niederhuber JE, Armitage JO, Kastan MB, Doroshow JH, Tepper JE, eds. Abeloff's Clinical Oncology. 6th ed. Philadelphia, PA: Elsevier; 2020:chap 71.
Shaheen NJ, Falk GW, Iyer PG, Gerson LB; American College of Gastroenterology. ACG clinical guideline: diagnosis and management of Barrett's esophagus. Am J Gastroenterol. 2016;111(7):1077. PMID: 26526079 pubmed.ncbi.nlm.nih.gov/26526079/.



Gastroesophageal reflux disease, or GERD, may have links to esophageal cancer. GERD is a condition in which stomach acid leaks into your esophagus, or food…

Norman Barrett isn’t a name that many people recognize. But there’s a well-known condition named for this Australian-born surgeon — Barrett’s esophagus. It refers to abnormal cell growth at the...